This editorial, written by Andréa Caprara and Valéry Ridde, was published last November in issue 23 of the Global Health Promotion magazine. It addresses the need to strengthen health promotion in Latin America through the example of the Zika epidemic. This article is also available in spanish, portuguese and in french.
Download and suggested citation:
As we celebrate the 30-year anniversary of the Ottawa Charter (1), the arrival of the Zika virus in Latin America and the declaration by the World Health Organization (WHO) of Zika as a global public health emergency at the end of 2015 remind us how little-known and little-implemented the Charter’s pillars are across the globe.
Over the last three years, Latin America has been confronted with different epidemics of viral diseases, all transmitted by the same vector, the Aedes aegypti mosquito. Latin American populations and health authorities have mainly been concerned with dengue, the most important viral infection in terms of its morbidity and economic impacts. In this context, the region also suffered the emergence of the Chikungunya virus in 2014, and then the Zika virus in 2015. Those charged with epidemiological surveillance at the local level no longer have space on their maps for new cases (Figure 1). This most recent epidemic became graver and more alarming when its potential correlation with a sharp increase in microcephaly and other congenital anomalies was found in fetuses and infants, suggesting vertical human transmission, as well as possible sexual transmission.
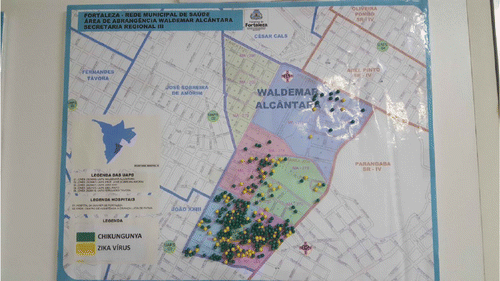
Figure 1. Map of the Waldemar Alcantara neighborhood in Fortaleza, Brazil, showing the location of cases of infection with Zika and Chikungunya viruses.
Often in the history of public health and disease control, the context of epidemics has been treated simplistically. Current debates seem focused on the quest for a miracle vaccine, despite the fact that the one recently introduced for dengue in Latin America is already being called into question (2). Calls for proposals for research focus on clinical and medical concerns, and less commonly on vector control interventions. It is surprising that evidence on the effectiveness and implementation of vector control interventions is so rare, given how long we have known about the role that these vectors play in disease transmission (3). Not all surveillance systems have integrated this new virus into mandatory reporting protocols. Furthermore, it seems that most interventions currently being implemented operate within a biomedical paradigm: aerial and land spraying of insecticide, transgenic mosquito release, installation of insecticide-treated bed nets, larvicide in water tanks, etc.
These avenues of research and intervention are useful and promising, even if systematically resorting to chemical insecticides is debatable for the environment and health. However, going ‘back to the future’ to a clinical and biomedical approach is worrisome. It is as if the Ottawa Charter of 1986 (1), the Sundsvall Declaration of 1991 (4), the ministerial declaration of Mexico City of 2000 (5), or the more recent conclusions and recommendations of the WHO Commission on Social Determinants of Health in 2008 (6) were once again completely forgotten. We will not go into the details of these declarations and the importance they give to the social determinants of health, to social inequalities in health (7) and to the ecological approach in health (8,9); however, the reactions to the arrival of the Zika virus in Latin America are telling, and reveal the need to affirm once again the values and actions upheld by health promotion. Research and training must be more interdisciplinary than they are today. The role of globalization, mass consumption, the dismantling of public services by a dominant neoliberal ideology and the rise of social inequalities in health in Latin America should all be priorities, not only for research but for action on epidemics like Zika.
Some may predict that the Zika epidemic will sputter out on its own and that the virus will not come back for several years; even so, we cannot stop intervening, because Aedes is responsible for other afflictions. For example, studies on the social determinants of dengue-related mortality are very rare (10) and more study in the social sciences needs to be undertaken on the social, human and psychological consequences of children with microcephaly. Intervention research using mixed methods to better understand interventions in their entirety needs to be funded. Ecological (11) and ‘biosafe’ (12) vector control programs should stop being studied only entomologically: they need to engage all disciplines to study interventions that are by their very nature complex. Participatory action research needs to be given more value by academia and by those who finance it (13), given that Latin American thinkers are its trailblazers (in particular Paolo Freire and Orlando Fals Borda).
The social sciences should be utilized to better understand interventions being implemented by national and local governments (9). Yet even if one of the rare courses on dengue in Latin America (http://www.redaedes.org) did choose to focus on Zika in 2016, not once during the four days of training was there a lecture on or reference to social science. The closing presentation mentioned no such avenue of research, only those concerning vaccination and biomedical aspects.
Initiatives at the local level also have to take the social determinants of health into account and work more intersectorally. Such collaboration would avoid creating further silos among health workers and vector control agents in cities, as well as urbanization and access to basic social services (education, contraception, etc.). The participation of populations, especially women (14), in the decisions that concern them, their family and their community, must once again be at the core of these actions, without falling into naïve optimism about certain approaches. Clinical research and vaccine development should certainly continue, but not at the expense of analyzing how health services can be reoriented toward primary care, the presence and training of qualified health personnel and the reduction of healthcare access inequalities for universal healthcare coverage (15).
The arrival (and soon the departure) of Zika in Latin America is a prime window of opportunity for political entrepreneurs in health promotion to raise their voices. Making themselves heard by ‘policy-makers [who] have had to make decisions in the presence of enormous uncertainty’ (16), on the other hand, is an entirely different matter! Nevertheless, we have to act now. Otherwise, Aedes and social inequalities will continue their destructive work.
References:
- Organisation mondiale de la santé (OMS). Charte d’Ottawa Pour la Promotion de la Santé. Ottawa: OMS; 1986. Accessible à : http://www.euro.who.int/__data/assets/pdf_file/0003/129675/Ottawa_Charter_F.pdf (consultè 24 août 2016). Google Scholar
- Halstead SB, Russell PK. Protective and immunological behavior of chimeric yellow fever dengue vaccine. Vaccine 2016; 34: 1643–1647. Google Scholar Medline
- Bowman LR, Donegan S, McCall PJ. Is Dengue vector control deficient in effectiveness or evidence? Systematic review and meta-analysis. PLoS Negl Trop Dis 2016; 10: e0004551. Google Scholar
- Organisation mondiale de la santé (OMS). Sundsvall Statement on Supportive Environments for Health. Rapport, 1991. Sundsvall: OMS. Accessible à : http://www.who.int/healthpromotion/conferences/previous/sundsvall/en/ (consultè 24 août 2016). Google Scholar
- Organisation mondiale de la santé (OMS). Rapport. Déclaration de México sur la Recherche en Santé. Rapport, 2000. México: OMS. Accessible à :http://www.who.int/rpc/summit/agenda/Mexico_Statement-French.pdf (consultè 24 août 2016). Google Scholar
- Organisation mondiale de la santé (OMS). Combler le Fossé en une Génération. Rapport final de la Commission des Déterminants Sociaux de la Santé, 2008. Genève: OMS.
- Ridde V. Reducing social inequalities in health: Public health, community health or health promotion? Promot Educ 2007; 14: 63–67. Google Scholar Abstract
- Charron DF. Ecohealth Research in Practice. Innovative Applications of an Ecosystem Approach to Health. Ottawa and New York: International Development Research Centre; Springer; 2012. Accessible à : http://www.deslibris.ca/ID/442211 (consulté 8 août 2016). Google Scholar
- Canadian Public Health Association (CPHA). Global Change and Public Health: Addressing the Ecological Determinants of Health. Rapport, 2015. Ottawa: CPHA.
- Carabali M, Hernandez LM, Arauz MJ, . Why are people with dengue dying? A scoping review of determinants for dengue mortality. BMC Infect Dis 2015; 15: 301. Google Scholar Medline
- Caprara A, Lima JW, Peixoto ACR, . Entomological impact and social participation in dengue control: A cluster randomized trial in Fortaleza, Brazil. Trans R Soc Trop Med Hyg 2015; 109: 99–105. Google Scholar Medline
- Bouyer J, Chandre F, Gilles J, . Alternative vector control methods to manage the Zika virus outbreak: More haste, less speed. Lancet Glob Health 2016; 4: e364. Google Scholar Medline
- Gilson L, Hanson K, Sheikh K, . Building the field of health policy and systems research: Social science matters. PLoS Med 2011; 8: e1001079. Google Scholar Medline
- Harris LH, Silverman NS, Marshall MF. The paradigm of the paradox: Women, pregnant Women, and the unequal burdens of the Zika virus pandemic. Am J Bioeth 2016; 16: 1–4. Google Scholar Medline
- Frenz P, Titelman D. [Health equity in the world’s most unequal region: A challenge for public policy in Latin America]. Rev Peru Med Exp Salud Pública 2013; 30: 665– 670. Google Scholar Medline
- Ferguson NM, Cucunuba ZM, Dorigatti I, . Countering the Zika epidemic in Latin America. Science 2016; 22: 353–354. Google Scholar
Trackbacks/Pingbacks